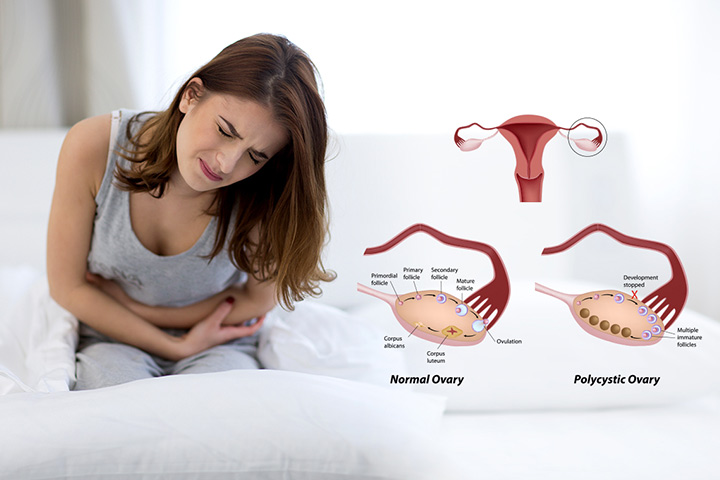
Polycystic Ovary Syndromes (PCOS) can be serious for some women: PMS, pelvic pain, acne, hair loss and infertility. Conception for a woman affected by PCOS can be difficult, but not impossible. Fertility doctors in America can help you start a family through reproductive medicine and technology.
When a woman does not ovulate, the doctor may first try fertility treatment. Clomid and Serophene, for example, can help trigger ovulation. If you have diabetes, you may also be prescribed Metformin to lower your insulin levels.
The most effective way to get pregnant for PCOS patients is IVF. In vitro fertilization is the combination of a woman’s egg and a man’s sperm outside the body. IVF requires a large number of doctor’s appointments, tests and injections, but all these inconveniences will be quickly forgotten once the baby is born!
A minimally invasive surgical procedure is also an option to stimulate ovulation. Your doctor may suggest a procedure called “ovarian drilling” in which the ovary receives a gentle electrical current. The effects may last several months, but it is important to discuss the risks involved with your doctor.
Your reproductive endocrinologist may also suggest some natural ways to help your body ovulate. Try to maintain a healthy weight and follow a healthy diet.
Choose foods that are unprocessed and contain as little sugar as possible, which will improve your insulin levels and hormone production. Exercise can also help.
Polycystic ovary syndrome has several serious complications.
Estrogen levels are high, increasing the risk of endometrial hyperplasia and ultimately endometrial cancer.
Androgen levels are often high, increasing the risk of metabolic syndrome and leading to hirsutism. Hyperinsulinemia due to insulin resistance may be present and may contribute to increased ovarian androgen production. In the long term, excess androgens increase the risk of cardiovascular disorders, including hypertension and hyperlipidemia.
The risk of androgen excess and its complications can be just as high in non-overweight women as in overweight women.
Recent studies indicate that polycystic ovary syndrome is associated with chronic low-grade inflammation and that women with polycystic ovary syndrome are at increased risk of non-alcoholic fatty liver disease.
Symptomatology
Symptoms of polycystic ovary syndrome usually begin during puberty and worsen over time. Premature adrenarche, characterized by excess dehydroepiandrosterone sulfate (DHEA) and often early growth of axillary hair, body odor, and microcomedonal acne, is common.
Characteristic symptoms include moderate obesity and hirsutism and irregular menstruation or amenorrhea. However, up to half of the women with polycystic ovary syndrome are of normal weight and some women are underweight. Body hair may grow in a male pattern (e.g., on the upper lip, chin, back, thumbs and toes; around the nipples and along the white line of the lower abdomen). Some women have other signs of virilization, such as acne and temporal baldness.
Other symptoms may include weight gain (sometimes difficult to control), fatigue, low energy, sleep problems (including sleep apnea), mood swings, depression, anxiety and headaches. In some women, fertility is impaired. Symptoms vary from woman to woman.
Areas of thickening, browning of the skin (acanthosis nigricans) may appear in the armpits, neck, in skin folds, and on the joints of the fingers and/or elbows, caused by high insulin levels due to insulin resistance.
If women with polycystic ovary syndrome become pregnant, the risk of pregnancy complications is increased, and complications are more severe if women are obese.
“These complications include gestational diabetes, premature delivery, and preeclampsia”, says Dr. Miguel Arruda, IVF specialist in Mexico.
Diagnosis
- Clinical Criteria
- Serum levels of testosterone, follicle stimulating hormone (FSH), prolactin, and thyroid stimulating hormone (TSH)
- Pelvic ultrasound
- Ovulatory dysfunction is usually present at puberty, causing primitive amenorrhea, so this polycystic ovary syndrome is probably not involved if regular menstruation has occurred for some time after menarche.
In polycystic ovary syndrome, the examination usually detects abundant cervical mucus, which is a reflection of estrogen levels. Polycystic ovary syndrome is suspected if patients present at least 2 typical symptoms.
Additional tests include a pregnancy test, measurement of serum testosterone, follicle stimulating hormone (FSH), prolactin and TSH; and pelvic ultrasound to rule out other possible causes of symptoms. Without serum testosterone is more sensitive than total testosterone but is technically more difficult to measure (see algorithm Diagnosis of Primary and Secondary Hypogonadism). Normal to slightly increased testosterone levels and normal to slightly decreased FSH levels suggest polycystic ovary syndrome.
Diagnosis requires at least 2 of the following 3 criteria:
- Ovulatory dysfunction causing irregular menstrual cycles.
- Clinical or biochemical signs of hyperandrogenism
- 10 follicles per ovary (detected by pelvic ultrasound), usually occurring at the periphery and resembling a pearl necklace
- In women meeting the criteria, serum cortisol is measured to exclude Cushing’s syndrome and serum 17-hydroxyprogesterone is measured early in the morning to exclude adrenal virilism. Serum DHEAS is measured. If DHEAS is abnormal, a test similar to amenorrhea is required.
Adult women with polycystic ovary syndrome are evaluated for metabolic syndrome by measuring BP and usually blood glucose and serum lipids (lipid profile).